Perimenopause and Oral Health: What Your Dentist Wants You to Know
Perimenopause and oral health are more closely linked than many women realise. As hormones fluctuate, changes in saliva, gum inflammation, tooth sensitivity and jawbone health can all become more noticeable. Yet many women are never told that symptoms such as bleeding gums, dry mouth or sensitive teeth may be connected to this stage of life.
If you’ve noticed bleeding gums, sensitive teeth, or a dry mouth that won’t go away, you’re not imagining it. This blog explains the connection between perimenopause and teeth, what’s happening biologically, and how a holistic dentist in Baker Street can support you through it.
What Is Perimenopause and Why It Affects Your Mouth
Perimenopause can begin as early as your mid-30s and often lasts several years before menopause. During this time, levels of oestrogen and progesterone fluctuate dramatically.
These hormonal shifts don’t just affect reproductive organs, they impact the entire body, including your mouth. Research shows that oral tissues and salivary glands contain oestrogen receptors, meaning they respond directly to hormonal changes.
This is why teeth in perimenopause can suddenly feel different, even if your oral hygiene hasn’t changed.
Common Oral Health Symptoms in Perimenopause
1. Dry Mouth (Xerostomia)
One of the most common complaints is persistent dry mouth. Up to 40% of menopausal women experience oral discomfort, including dryness, burning, or sensitivity. [1] Oestrogen helps regulate saliva production, so when levels drop, saliva decreases.
Why this matters:
- Saliva protects teeth from acid and bacteria
- It helps remineralise enamel
- It reduces risk of decay
Reduced saliva increases your risk of cavities and gum disease.
2. Sensitive Teeth
If hot drinks or cold foods suddenly cause discomfort, you’re not alone. Many women report increased tooth sensitivity during perimenopause.
This is often linked to:
- Reduced saliva protection
- Enamel wear
- Gum recession exposing dentine
Hormonal changes don’t directly damage enamel, but they create conditions where damage happens more easily.
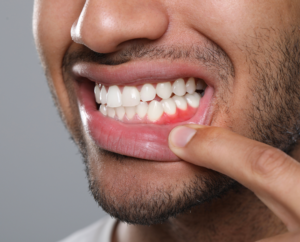
3. Bleeding or Inflamed Gums
Hormonal fluctuations can make gums more reactive to plaque bacteria. This condition, sometimes referred to as menopausal gingivostomatitis, can cause:
- Red, swollen gums
- Bleeding when brushing
- Increased tenderness
This is similar to pregnancy gingivitis, another hormone-driven oral condition.
4. Increased Risk of Gum Disease
Gum disease (periodontitis) becomes more common during perimenopause and beyond. Chronic inflammation combined with reduced immune response can accelerate gum breakdown.
Studies suggest women in menopause are at higher risk of oral health problems and unmet dental needs, highlighting a gap in awareness and care.[2]
5. Bone Loss and Tooth Stability
Oestrogen plays a key role in maintaining bone density, including the jawbone that supports your teeth. After menopause:
- Bone mineral density declines
- Risk of tooth loss increases
- Periodontal disease progression can accelerate
Research links lower bone density with increased tooth loss in postmenopausal women.
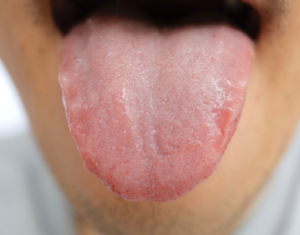
6. Burning Mouth Syndrome & Taste Changes
Some women experience:
- Burning sensations in the tongue or lips
- Metallic or altered taste
- Tingling or discomfort
These symptoms are strongly associated with hormonal fluctuations and reduced saliva.
Why Many Women Are Not Told About This
Despite growing evidence, awareness remains low. A 2025 integrative review found:
- Limited knowledge among women about menopause-related oral health
- Inconsistent advice from healthcare providers
- Lack of clear guidelines for dental professionals
This means many patients only discover the link between perimenopause and oral health after symptoms appear.
The Mouth–Body Connection: A Holistic Perspective
Your oral health is not separate from your general health. Hormonal imbalance, inflammation, nutrition, stress, and sleep all play a role. A 2025 integrative review found most women had limited awareness of menopause-related oral health risks, and healthcare guidance was inconsistent. [3]
A holistic dentist in Baker Street will look beyond the teeth and gums to understand:
- Hormonal status
- Nutritional deficiencies (e.g. vitamin D, calcium)
- Lifestyle factors
- Systemic inflammation
This whole-body approach is particularly important during perimenopause, when multiple systems are changing at once.
What You Can Do: Practical Steps to Protect Your Teeth in Perimenopause
1. Prioritise Preventive Dental Care
Regular hygiene visits and check-ups are essential. Early intervention can prevent long-term damage.
2. Support Saliva Production
- Stay well hydrated
- Reduce caffeine and alcohol
- Use saliva-supporting products if needed
3. Upgrade Your Oral Hygiene Routine
- Brush twice daily with a remineralising toothpaste, and speak to your dental team about the best option for your risk profile.
- Floss or use interdental brushes daily
- Consider products for sensitive teeth
4. Focus on Nutrition
Support both oral and bone health with:
- Calcium
- Vitamin D
- Magnesium
- Omega-3 fatty acids
5. Manage Hormonal Health
Work with a healthcare provider to explore options such as:
- Lifestyle changes
- Nutritional support
- Hormone replacement therapy (if appropriate)
6. Address Gum Health Early
Bleeding gums are not “normal”, they are an early warning sign. Treating inflammation early can prevent bone loss.
Why See a Dentist Who Understands Perimenopause?
Not all dentists are trained to recognise the link between perimenopause and teeth. A dentist with experience in this area can:
- Identify early hormonal signs in the mouth
- Personalise your preventive care plan
- Work alongside other healthcare providers
- Support long-term oral and systemic health
If you’re searching for a dentist in Baker Street who understands these changes, choosing a holistic approach can make a significant difference.
Meet Our Holistic GP: Sonia Tsukagoshi

At our clinic, we take an integrated approach to women’s health. That’s why we work closely with our in-house holistic GP, Sonia. Sonia has a special interest in:
- Perimenopause and menopause care
- Hormonal balance and optimisation
- Functional and lifestyle medicine
- Nutritional support for whole-body health
- Longevity and whole-body health
By combining dental care with medical insight, we can address the root causes of symptoms, not just the surface effects. This collaborative approach ensures that your oral health, hormones, and overall well being are treated together, not in isolation.
Don’t Ignore Changes in Your Mouth
Perimenopause is a natural phase, but the symptoms can feel anything but.
If your teeth feel more sensitive, your gums are bleeding, or your mouth feels dry, these are not random changes. They are signals from your body.
The good news? With the right care, support, and awareness, you can protect your smile and your health for years to come. To book a 15-point dental health check, call us today on 020 3921 1000 or email hello@optimaldental.co.uk. Click here to find out what to expect as a new patient.
About the Author, Dr James Goolnik

Dr James Goolnik is a holistic dentist in Baker Street and founder of Optimal Dental Health, with over 30 years of clinical experience. He is known for his integrative approach, combining advanced dentistry with nutrition, lifestyle medicine, and whole-body health.
He has a special interest in the link between oral health and systemic conditions, including how perimenopause and menopause affect teeth and gums. Dr Goolnik works with patients to identify root causes of oral health issues, not just treat symptoms.
He has completed extensive postgraduate training in functional medicine and preventive dentistry, and is a certified practitioner with the Institute for Functional Medicine (IFM).
Dr Goolnik is committed to helping patients understand the connection between their oral health and overall wellbeing, offering personalised, evidence-based care as part of a multidisciplinary team.