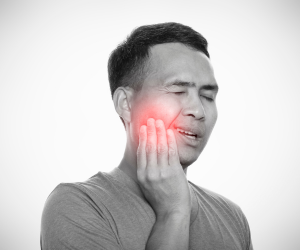
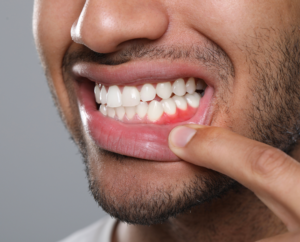
What is a Dry Socket? Symptoms, Causes & When to Worry After Tooth Extraction
If you’ve recently had a tooth removed, it’s completely normal to have questions about healing and recovery, especially if you’re experiencing discomfort afterwards.
One of the most common concerns patients ask us about is dry socket after tooth extraction. Many of you wonder:
“How do I know if I have a dry socket?”
“What does a dry socket feel like?”
“When should I worry?”
At Optimal Dental Health, we understand that healing after a dental extraction can feel overwhelming, particularly if pain suddenly increases after a few days. Our aim is always to help you feel informed, reassured and fully supported throughout your recovery.
In this guide, we explain:
- What a dry socket is
- Common dry socket symptoms
- When to worry about a dry socket
- What causes a dry socket
- How is a dry socket treated
- How a holistic approach may help support healing after extraction
What is a Dry Socket After Tooth Extraction?
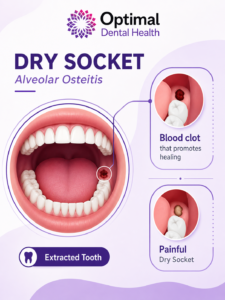
A dry socket, also known clinically as alveolar osteitis, is one of the most common complications that can occur after a tooth extraction.
Normally, after a tooth is removed, your body forms a protective blood clot inside the socket. This blood clot acts like a natural bandage, protecting the bone and nerves underneath while new tissue heals over the area.
A dry socket happens when:
- The blood clot becomes dislodged too early
- The clot dissolves prematurely
- Or the clot never properly forms
When this happens, the underlying bone and nerve endings become exposed, which can lead to significant pain and delayed healing.
Dry socket most commonly occurs after wisdom tooth extractions, although it can happen after any extraction procedure.
According to the NHS and oral surgery literature, dry socket affects approximately 1–5% of routine extractions, but the risk increases after surgical wisdom tooth removal. [1]
Dry Socket Symptoms: How Do I Know If I Have a Dry Socket?
One of the most common questions we hear is: “How do I know if I have a dry socket?” The symptoms are usually quite distinctive and often begin between 1 to 5 days after your extraction. Common dry socket symptoms include:
Increasing or Severe Pain
Instead of gradually improving each day, the pain suddenly becomes worse. Many patients describe it as throbbing, deep or radiating pain.
Pain Spreading to Other Areas
The discomfort may spread to your ear, jaw, temple, eye or neck. This radiating pain is one of the hallmark symptoms of dry socket.
An Empty-Looking Socket
You may notice that the extraction site looks hollow or empty instead of containing a dark blood clot. You may even see a small section of exposed bone.
Bad Taste or Bad Breath
A dry socket often causes an unpleasant taste or smell that does not improve with brushing or improving your oral health routine.
Painkillers Not Working Properly
You may notice that standard pain relief offers very little relief once a dry socket develops. Importantly, normal extraction discomfort should gradually improve every day. If your pain is worsening instead of improving, this is often the biggest warning sign.
Normal Healing vs Dry Socket: What’s the Difference?
It can sometimes be difficult to know what is considered normal after an extraction.
Normal Healing After Extraction
You may experience:
- Mild to moderate discomfort
- Swelling
- Tenderness
- Slight bleeding in the first 24 hours
- Gradual improvement each day
Dry Socket Symptoms
You may notice:
- Pain becoming worse after 2–3 days
- Sharp or throbbing pain
- Pain radiating to the ear or jaw
- Foul smell or taste
- Visible empty socket
If you are ever unsure, it is always best to contact your dentist in London for expert advice.
When to Worry About a Dry Socket
So, when should you worry about a dry socket? You should contact your dentist if:
- Your pain becomes significantly worse after day 2 or 3
- You notice a foul smell or taste
- Pain relief is no longer helping
- You think the blood clot may have become dislodged
- You can see exposed bone
- You are struggling to sleep because of the pain
Although dry socket is not usually dangerous, it can be extremely uncomfortable and may delay healing if left untreated. At Optimal Dental Health, we always encourage you to contact us early if something doesn’t feel right. Prompt care can make a significant difference to your comfort and healing.
What Causes Dry Socket After an Extraction?
There is rarely one single cause. Usually, several factors contribute to the clot becoming disrupted. Common dry socket risk factors include:
Smoking or Vaping: Smoking is one of the biggest risk factors because it reduces blood flow and healing capacity while the suction can dislodge the clot.
Drinking Through a Straw: The suction created can disturb the blood clot.
Vigorous Rinsing or Spitting: This can physically dislodge the clot during the early healing stages.
Difficult or Surgical Extractions: More traumatic extractions naturally increase inflammation and healing demands.
Poor Oral Hygiene: Bacteria around the extraction site may interfere with healing.
Hormonal Factors: Some studies suggest a slightly increased risk in patients taking oral contraceptives.
Certain Medications: Medications affecting blood clotting or immune response may influence healing. [2]
A Holistic Approach to Healing After Tooth Extraction
At Optimal Dental Health, we take a holistic approach to recovery after extractions and oral surgery. This means we do not just focus on the tooth itself, we consider your nutrition, immune health, inflammation, stress levels, sleep, lifestyle factors and whole-body healing capacity.
Our goal is always to support the body’s natural healing processes as gently and effectively as possible.
Before Your Extraction
We may recommend:
- Optimising your vitamin C intake
- Ensuring adequate protein intake
- Supporting vitamin D levels
- Staying well hydrated
- Reducing smoking or vaping where possible
- Managing stress and sleep
After Your Extraction
We advise:
- Avoiding straws, smoking and vigorous rinsing
- Eating soft, nourishing foods
- Resting properly
- Following all aftercare instructions carefully
- Supporting the oral microbiome during healing
- Avoiding mouthwash
We may also recommend supportive therapies such as:
- Ozone therapy
- PRF (Platelet Rich Fibrin)
- Nutritional support where appropriate
Ozone Therapy and Healing Support
At Optimal Dental Health, we often incorporate ozone therapy as part of our holistic surgical protocols. Ozone therapy is used in dentistry for its antibacterial properties and anti-inflammatory support. [3]
It can also support tissue healing and reduce harmful bacteria within the socket. You can learn more about our Ozone Therapy in London here.
What Happens If You Have a Dry Socket?
If we suspect a dry socket, treatment is usually very straightforward and focused on relieving discomfort and supporting healing. Treatment may include:
- Gently cleaning the socket
- Removing debris
- Applying a soothing medicated dressing- like Alveogyl
- Providing targeted pain management advice
- Monitoring healing progress
You will begin to feel significant relief within 24-72 hours after treatment. You can find out more about our emergency dental appointments here.
How Long Does a Dry Socket Last?
Without treatment, dry socket pain may last around 7–10 days or sometimes longer. With prompt professional care, symptoms often improve much faster and healing can continue more comfortably. Every patient heals differently, which is why personalised care is so important.
Frequently Asked Questions
What is a dry socket in simple terms?
A dry socket is when the protective blood clot after a tooth extraction becomes dislodged or fails to form properly, exposing bone and nerves.
How do I know if I have a dry socket?
Pain that gets worse after a few days instead of improving is one of the biggest warning signs.
Are dry sockets common?
They are relatively uncommon but are more likely after wisdom tooth removal, lower teeth extractions or in smokers.
Can dry socket heal on its own?
Yes, but professional treatment usually relieves pain much faster and supports smoother healing.
Can antibiotics treat dry socket?
If severe they can help, look out for a temperature or facial swelling. Best to clean the area out and encourage the formation of a blood clot.
How can I reduce my risk of dry socket?
Avoid smoking, straws, forceful rinsing and disturbing the extraction site. Following your aftercare instructions carefully is the best prevention.
Prompt Care Supports Faster Healing
Understanding what a dry socket is, recognising the symptoms early, and knowing when to seek help can make a significant difference to your recovery after a tooth extraction.
If you are worried about pain, healing or symptoms after an extraction, please do not hesitate to contact us. Early support can help relieve discomfort quickly and support smoother healing. We provide treatments to support you, including the Septodont dry socket surgical dressing.

At Optimal Dental Health, we are here to guide you through every stage of your dental journey with a gentle, holistic and patient-centred approach to care.
To book an appointment or speak to our team:
Call us on 020 3921 1000
Email hello@optimaldental.co.uk
Or visit www.optimaldentalhealth.co.uk
About the Author: Dr James Goolnik

This article has been written and clinically reviewed by Dr James Goolnik, Director of Optimal Dental Health, London. Dr Goolnik has over 20 years of clinical experience in cosmetic, restorative and holistic dentistry and is widely recognised for his minimally invasive and whole-body approach to oral health.
Dr Goolnik is registered with the General Dental Council (GDC) and is a leading advocate for patient-centred holistic dental care in the United Kingdom. Visit his website here.